Claim adjudication is a crucial review process in medical billing, acting as a bridge between healthcare providers and payers. It determines how a claim is processed and handled post-submission to the payer.
Understanding this process helps ensure timely reimbursements and plays a significant role in improving the overall efficiency of the healthcare revenue cycle. It also ensures:
- Improved provider financial stability
- Enhanced quality assurance
- Reduced errors
- Better data utilization
- Increased patient satisfaction
However, claim adjudication is only effective when billing professionals and payers clearly understand the process. In this article, we will:
- Discuss the importance of medical claims adjudication
- The steps in the process
- Address the challenges faced
- Offer suggestions for improvement
- Review the latest software solutions available in 2026
Steps Involved in the Claim Adjudication Process
According to Becker’s Hospital Review in 2024, 46% of respondents said missing or inaccurate data is one of the top three reasons for denials. Many times, payers detect inaccuracies in the claim information during the initial review and reject the claim, disrupting the healthcare provider’s revenue cycle.
But how does claim adjudication work in medical billing? Here’s a comprehensive breakdown of the process and what each step entails.
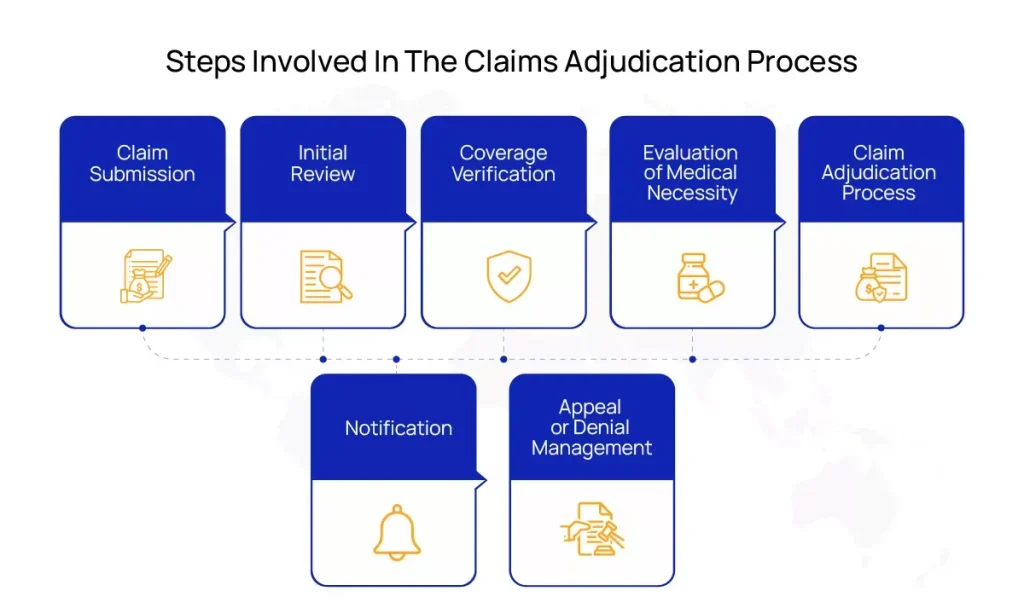
| Steps Involved | Description |
|---|---|
| Claim Submission | The medical service provider submits the claim containing the pertinent patient information, necessary documentation, and services rendered. |
| Initial Review | The insurer performs a preliminary check to ensure all the documentation is complete and accurate. Here, they may request additional documents (if applicable). This can be done manually by the team or by leveraging billing software to tackle human errors. |
| Coverage Verification | The payer checks the insurance validity and coverage limits to determine which services are covered under the patient’s insurance plan. |
| Evaluation of Medical Necessity | The payer assesses the claim according to the latest guidelines to determine whether the services rendered meet requirements for medical necessity. |
| Final Determination | The insurance payer determines the claim’s final status. Here, a claim can be accepted, rejected, or partially approved. |
| Notification | An Explanation of Benefits (EOB) is sent to the patient, or a Remittance Advice (RA) is sent to the medical service provider, listing services covered under the policy terms, or the reason for a claim denial. |
| Appeal or Denial Management | The provider can rectify errors, provide supplementary information, and resubmit the request to address and resolve the denial. |
Note: Generally, all steps before final determination are considered pre-adjudication steps, while notification and appeals are post-adjudication activities. You can find additional tips for managing denials here.
Challenges with the Claim Adjudication Process
Claim adjudication is a complex process and presents several operational challenges. The following are some common challenges that arise:
Complex and Changing Regulations
Changing healthcare regulations often confuse medical billing teams, leading to inaccuracies. Therefore, billing teams should be aware of the latest guideline changes and regulation updates.
Varying Payer Requirements
Payers such as Medicare are not the only ones providing medical coverage to patients. Patients may have coverage from several private insurers, each with their own policies and guidelines.
A large number of payer-specific requirements makes it challenging for billing teams to submit a clean claim.
Massive Claim Volume
A high volume of claim submissions is overwhelming for the processing staff, especially in cases where the submitted claims have short deadlines. Similarly, professionals may rush the claim process to meet deadlines, resulting in errors and inaccuracies due to human limitations.
Denial Management
Submitting a denial appeal can prolong the reimbursement cycle, posing a serious challenge for medical billers. It is time-consuming and labor-intensive, resulting in massive bottlenecks in the process.
Technological Limitations
Not every healthcare practice has access to software and digital tools for billing. Therefore, claims submitted manually are generally less effective and have a high chance of errors. Medical billing teams should adopt the right medical claims adjudication software moving forward. But this must be done after careful consideration.
How to Improve the Claim Adjudication Process?
The average time for claim adjudication in medical billing is between 14 and 30 days. It means that if the claim is error-free and meets the payer’s reimbursement guidelines, it can be processed and paid within a few weeks. Otherwise, it could take a couple of months or even stretch to 180 days if denied.
This is a long period, leading to revenue bottlenecks for medical service providers and disrupting patients’ treatment in some cases. Therefore, providers must know how to improve the claim adjudication process, and it can be done by using the following steps:
Submit Complete Claims
Adding precise and complete details is necessary when billing the payer. In most cases, your reimbursement request will be accepted immediately if it fulfills the latest requirements and follows the prescribed guidelines.
However, if you face challenges with submitting your claims, review the guidelines, rectify claim errors, and resubmit the request.
Train Billing Staff
A trained billing staff is the foundation of seamless claim adjudication. Your system will only be as efficient as your team; therefore, you should invest in them. The billing team should know the latest guidelines and applicable changes. Ideally, your staff should know the:
- Latest coding standards
- Medical necessity guidelines
- Payer policies
Conduct Regular Audits
Oftentimes, billing systems are not working optimally because the medical facility has not identified the shortcomings or gaps in the system. Thus, we recommend conducting regular system audits and identifying potential errors to streamline the billing process.
Build and Maintain Professional Relationships with Payers
The payer plays a vital role throughout the billing process and dictates several policies. For instance, the AAPC states that:
If a payer stipulates a 90-day timely filing requirement, it means the claim must be submitted within 90 days from the date of service.
These guidelines and regulations might change annually, making it challenging for professionals to keep up with them. But when service providers have a strong professional relationship with the insurance company, they can discuss denials and learn the triggers. Hence, it becomes easier to meet the payer’s specific requirements and enjoy the fruits of successful claim adjudication.
Implement Standardized Practices
Consistency is key to accurate billing. Therefore, your team should adopt a standardized policy to achieve accuracy inherently.
For instance, it may include double-checking the latest document requirements per the payer’s policy manual or scrubbing the claim before submission.
Educate Patients
In some cases, medical billing delays and rejections can also occur because patients do not fully understand how billing works or end up conveying incorrect or outdated information to the provider.
Fortunately, educating patients regarding billing concepts like ‘coordination of benefits’ and ‘out-of-pocket’ costs can greatly reduce confusion and billing disputes. We also recommend educating patients about denials because of their mistakes to ensure they understand their role in the billing process.
Utilize a Billing Software
Human error may remain a consistent part of medical billing, but this can be countered by leveraging the right billing software. These solutions offer various useful features, such as:
- Error detection
- Real-time eligibility checking
- Comprehensive reporting
These features help healthcare providers rectify mistakes before submission, drastically improving the rate of claim acceptance.
Software for Medical Claims Adjudication in 2026
Selecting the right software for claims adjudication in medical billing can be a massive game-changer for providers. Here are some popular software to review before choosing one:
| Adjudication Software | Key Differentiator (USP) |
|---|---|
| MedCare MSO | Utilizes the latest AI automation for faster, accurate billing cycles. |
| CollaborateMD | Suitable for diverse operational needs. |
| Tebra | Smoothly integrates patient engagement and billing features. |
| EZClaim | Simple, efficient, cost-effective, and user-friendly platform. |
| eClinicalWorks | Offers lower denial rates because of an automated checking system. |
| Athenahealth | Network-driven billing, resulting in smarter and higher collections. |
| AdvancedMD | Ideal for practices seeking growth and expansion because of scalability options. |
| NextGen Healthcare | Easy-to-use financial analytics and reporting tools. |
| RXNT | Combines billing and scheduling capabilities through its comprehensive platform. |
NeuraBill Eases Claim Adjudication in Medical Billing
To recap, claim adjudication helps determine the outcome of a submitted claim, whether a claim will be accepted, adjusted, delayed, or denied. The decision depends on the payer’s latest guidelines and the provider’s compliance with them.
We recommend reviewing the medical claims adjudication software we mentioned in this blog to pick the right one. However, if you still receive denials due to errors, consider acquiring third-party denial management services, such as those offered by NeuraBill.



